Zinc is an essential micronutrient involved in the metabolism of enzymes, proteins, carbohydrates and vitamins [1]. It also plays an important role in the defence mechanisms against pathogens [2, 3]. A decreased level of zinc causes a rare disease – acrodermatitis enteropathica (AE). There are two forms of this disorder: primary and acquired. The autosomal recessive mutations in the SLC39A4 gene, which encodes a transmembrane zinc transporter protein is a cause of the primary form and the diagnosis is made in newborns [4, 5]. The acquired form is caused by malabsorption or a low amount of this micronutrient in the diet and can be diagnosed at any age [5]. High alcohol intake is one of the causes of the acquired AE [3, 6, 7].
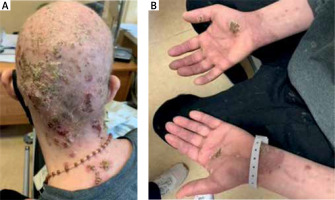
A 28-year-old patient was admitted to the dermatological department in March 2021. The patient presented with hyperkeratotic, partly psoriasis-like lesions located on his hands, feet and scalp and erythematous, scaly lesions noticed around periorificial areas. Additionally, physical examination revealed significant hair loss (Figures 1 A, B). The lesions were infected and partially covered with a honey-like crust. The clinical picture and social history of the patient, which included homelessness, high alcohol intake and smoking led to the decision to request a laboratory test for the serum zinc level. The test revealed that the serum zinc level was significantly below the normal range, at 33 μg/dl (66–110.0 μg/dl). The blood tests also showed mild anemia, elevated C-reactive protein (CRP) and hypoalbuminemia. Serum levels of potassium, sodium and chloride were within normal ranges. Bacterial culture from the skin lesions grew Staphylococcus aureus. Based on the clinical picture and the results of the laboratory tests, acrodermatitis enteropathica was diagnosed. The most likely reason for the decreased level of zinc was excessive alcohol intake and reduced amount of zinc in the diet. Oral supplementation with 150 mg of zinc hydrogen aspartate twice a day was started. In addition, due to the secondary bacterial infection, systemic (i.v.) ceftriaxone was prescribed. The skin condition and zinc level gradually improved. The patient was discharged after 10 days with a recommendation to continue oral zinc supplementation. Discontinuation of alcohol consumption was also recommended to the patient.
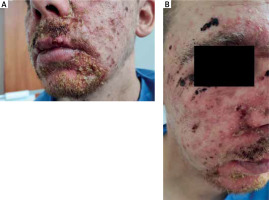
The patient was readmitted to the hospital in September 2021. He did not supplement zinc after discharge. Clinical examination showed signs of bacterial infection on top of dermatological lesions which were similar to those seen previously. Again, large areas of honey-coloured crusts were noticed on the patient’s face (Figures 2 A, B). Moreover, the patient complained of recurrent diarrhoea. Laboratory tests revealed low levels of zinc, at 28 μg/dl, elevated levels of alanine transaminase, aspartate transaminase, CRP, and white blood cells count with anemia and hypochloridaemia also present. Treatment with systemic ceftriaxone, oral prednisone and diazepam with supplementation of vitamins B, vitamin C and iron was started. Oral zinc supplementation with 150 mg of zinc hydrogen aspartate twice a day was resumed. The patient’s skin symptoms gradually improved with face and scalp lesions resolving first. Laboratory test results were back to normal within 20 days with the zinc level reaching 82 μg/dl. The patient was discharged from the hospital with an emphasis on a strong regomendation of regular supplementation of zinc. The patient did not attend any follow-up visits, most likely due to his social circumstances.
Figure 2
A, B – Honey-coloured crusts located on the patient’s face due to secondary bacterial infection
Typically patients with AE present with signs of a classical triad: (1) psoriasis-like dermatitis on the limbs coexisting with (2) alopecia and (3) diarrhoea [6, 8, 9]. The patient described in our case report presented with all of the classical AE’s triad symptoms – alopecia, acral lesions and diarrhoea, however the last one did not appear during his first admission. Anemia which was present in our patient, was described in other reports of AE [6].
Zinc is involved in mechanisms against pathogens by promoting T-helper cells which are taking part in cell-mediated immune mechanisms against bacteria, such as Staphylococcus aureus [10]. Therefore, bacterial infections often occur in patients with acrodermatitis enteropathica. Our patient had secondary infection with Staphylococcus aureus, which manifested as honey-coloured crusts.
The diagnosis of acrodermatitis enteropathica is made on clinical findings and low serum zinc levels. In unclear cases histopathology of the skin may be helpful [5]. Our patient presented with all typical symptoms of AE and crucially the serum zinc level was below normal level.
The treatment of choice in acrodermatitis enteropathica is zinc supplementation, which leads to remarkable clinical improvement [6, 8, 9]. The recommended starting dose of zinc is 3 mg/kg/day of elemental zinc, with preference of oral over parenteral supplementation [5, 8, 9]. After the implementation of zinc, patients with AE tend to improve within a short time, usually 1 to 2 weeks, as it was noticed in our patient [6, 8, 9]. It is recommended to measure the level of zinc every 3–6 months [11]. Therapy with zinc leads to 100% response in treated patients. Stopping zinc supplementation can lead to recurrence of the disease and even premature death [5]. This case proves how important the continuous zinc supplementation is in the patients with acrodermatitis enteropathica. The condition of our patient deteriorated dramatically after the discontinuation of the treatment and readmission of the patient was necessary.